by Drs. Shobha Ravishankar, Normals S. and Dr. So am Nisar Chennai
Abstract
Children with cranio-facial abnormalities provide a challenge to anaesthesiologists as management of a paediatric airway in such cases is difficult. Airway difficulty should be anticipated and a plan to manage untoward events should be ready during preoperative evaluation. It is important to understand the development and characteristics of the anomalies and their peculiar anaesthetic challenges in order to plan a safe anaesthetic. A rarest of rare case is described here which was successfully dealt with in our hospital. The literature description of Tessiers Type 2 is sparse.
Key words: Difficult airway, Orofacial clefts, Tessiers type 2 cleft
Introduction
Oro-facial clefts are among the rarest of malformations with an incidence of 1.43-4.85 per 100’000 births and 1% among children born with cleft lip and/or cleft palate (788997). Surgical treatment of these cranio-facial abnormalities is a challenge not only to anaesthetists but also for the surgeon. The successful management of this rare case is described here.
Case Report
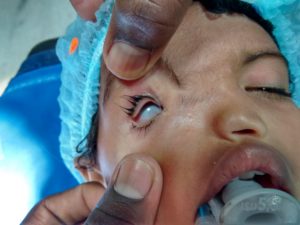
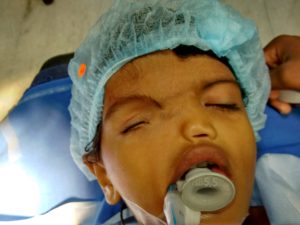
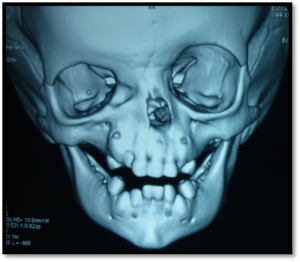
A one year old female child weighing 8 kilograms in ASA I group was scheduled for Dacro-Cysto-Rhinostomy of the right side under general anaesthesia. The child was diagnosed as Tessier’s type 2 anomaly but had no other associated congenital anomalies. On examination she had right anophthalmus and right side arhinia. Systemic examination and haematology were unremarkable.
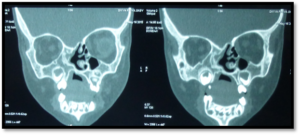
Fig
MRI picture showing right arhinia
Anaesthetic Management
The child was kept nil per mouth as per universal guidelines. Difficulty in mask induction was anticipated because of gross facial dysmorphism.
The baby was premedicated with i.m. glycopyrrolate 45 minutes preoperatively. Baby was induced with O2, N2O and Sevoflurane. To achieve tight fit for face mask, adequate folded gauze was used and the airway was kept patent using Guedel’s oral airway. With this the spontaneous bag movements were adequate and peripheral oxygen saturation maintained 100%.
I.v. fentanyl 1 mcg/kg was given for analgesia. Baby’s ventilation was assisted manually and after adequate depth was ensured, a trail laryngoscopy was performed. With deep cricoid pressure posterior cords were visualised and the trachea was intubated with 4mm uncuffed endotracheal tube. The oral cavity was packed to ensure there was no air leak. The baby was paralysed by giving Atracurium 0.5 mg/kg body weight. Intra operatively baby was monitored with ECG, NIBP, SPO2, and capnography. Vitals were well maintained throughout the procedure. The residual paralysis was reversed with neostigmine and glycopyrrolate at the end of the procedure. The child was extubated awake and monitered in PACU.
Fig
Discussion
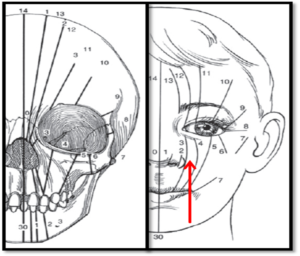
Tessiers in 1976 classified cranio facial clefts according to anatomical defects as facial, cranio-facial and latero- facial and numbered them from 0-14.
Tessiers clefts
The causative factor is still unclear. It is possible that these malformations are caused by a disorder in the migration of neural crest cells (12900623). Another theory is failure of fusion processes and failure of inward growth of mesoderm. Tessiers number 1,2,12 and 13 are paramedian clefts. They are similar to midline clefts but farther away from midline of face. Tessiers 1 and 2 both come through maxilla and nose in which Tessiers 2 is further from midline than Tessiers 1.
The main challenge in anaesthetic management is to maintain airway patency (8275642). Airway problems in children with such gross craniofacial abnormalities is well recognized. Thus a prudent preoperative plan for the conduct of anaesthesia is mandatory. Induction can be difficult as mask fit is a challenge.
Conclusion
A proper stepwise planning is a must for a safe conduct of anaesthesia in such cases.
(8679343)