Dr. Shoba Ravishankar
Consultant Anaesthetist
Department of Anaesthesia
No 6, College Road, Nugambakkam
Sankara Nethralaya
Chennai India
Key words: Epibulbar dermoid, Oculoauriculovertebral dysplasia, Difficult intubation
Introduction
Goldenhar Sydrome is a genetic disorder, with autosomal dominant inheritance and with an incidence of 1:3000 –1:5000 with a Male: female ratio of 2:1. It was first described by Goldenhar in 1952. It is characterized by asymmetry which can be unilateral (hemi facial microsomia) (17315807) or bilateral in 10-33% of cases. The right side of the face is more affected with a sporadic or familial occurrence.
Case History
A five year old female child weighing 15 kgs was posted for coloboma repair of both upper eyelids. The birth history and the neonatal period was uneventful. The patient was referred to our tertiary centre because of history of failed intubations (3241587) twice.
Physical examination
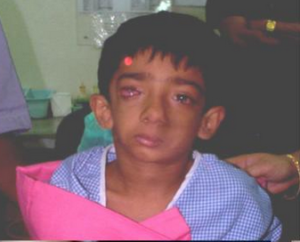
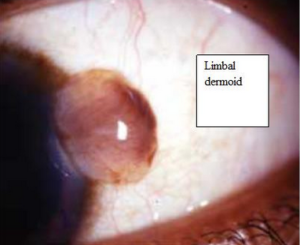
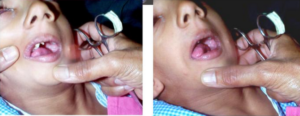
On clinical examination, the patient had marked facial asymmetry with micrognathia, mandibular hypoplasia, dental malformation, preauricular skin tags, coloboma of both upper eyelids & limbal dermoid (19783022). The patient also had a clefting of the right half of the tongue. The airway was graded as Mallampatti III and thus a difficult intubation was anticipated. The cardiovascular and respiratory system were found to be within normal limits.
Investigations
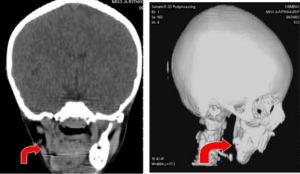
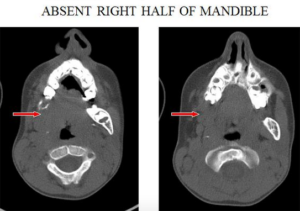
The routine haemogram and coagulation profile were within normal limits. The X ray of the cervical spine showed hemi-vertebrae with increase in the atlantoaxial distance. The chest Xray PA view showed trachea to be in normal position. CT scan mandible revealed absence of the right half of the mandible.
Anaesthetic Management
Since the child had a previous history of difficult airway, we planned for a trial laryngoscopy under inhalational anaesthesia. The child was premedicated with Inj.Glycopyrrolate 0.002mg/kg IM 45 minutes preoperatively. Induction was carried out with O2, N2O (50:50) and sevoflurane 6% concentration using Jackson’s Rees Circuit. Intravenous access was secured and 0.45%Dextrose normal saline was started. Following bag-mask ventilation for three minutes, trial laryngoscopy by left molar (19234820) approach was performed. The vocal cords were visualized and hence the child was paralysed with the non-depolarising muscle relaxant Inj.Rocuronium 0.6mg/kg. IV. The child was intubated with 5mm ID portex plain endotracheal tube (ETT). After confirming the placement of the tube with bilateral equal air entry on auscultation and with End-tidal CO2 tracings maintaining between 20-30mmof Hg, ETT was secured. The oro-pharynx was packed with sterile wet gauze. Injection Fentanyl 1mcg/kg was administered intravenously for analgesia.
The intraoperative vital signs were within normal limits. The surgical procedure lasted for about two and half an hour. At the end of the surgery the residual neuromuscular block was reversed with Inj.Neostigmine 0.5mg/kg and Inj. Glycopyrrolate 0.005mg/kg IV.
The patient was extubated completely awake with intact reflexes. The child was shifted to post anaesthetic care unit and was monitored with ECG, SpO2 and NIBP for two hours.
Discussion
A variety of terms have been used to describe this extremely variable disorder. According to medical literature when malformation primarily involve only one side of the jaw, mouth, eyes it is called as ‘Hemifacial Microsomia’. If abnormalities of eyes and vertebrae are also present it is called as ‘Golden har Syndrome’. Though this syndrome is described by different names, it has been suggested that these entities may represent gradations in severity of errors in morphogenesis.
Golden har syndrome has various synonyms like- Oculoauricular vertebral dysplasia, Oculoauriculo vertebral syndrome,Facioauriculo vertebral anomaly syndrome, First and second branchial arch syndrome.
It is also seen as a common association with CHARGE
- Coloboma of choroid
- Heart defect
- Atresia of choana
- Retarded growth
- Genital hypoplasia
- Ear anomalies/ deafness
Goldenhar syndrome is the second common facial defect known. Principal facial deformity of the syndrome is focused on oto- temperomandibular region, then radiates circumferentially to involve middle and lower two-thirds of facial skeleton and overlying soft tissue.
A combination of several features such as microtia, hemifacial microsomia, lateral facial cleft, epibulbar dermoid and upper eye lid coloboma is seen.
Pathogenesis
The exact cause is not known. The possible causes as described by Stark and Saunders could be disturbed neural crest development, deficiency in migration of neural crest cells, deficiency of mesodermal formation or defective interaction between neural crest cells and mesoderm.
The second theory of pathogenesis states the possible causes to be vascular disruption in the region of first and second branchial arches (Poswillo 1973) or Infants of diabetic mothers are at increased risk of OAVS (Wang et al 2002).
Associated features of this syndrome include
- Thyroid abnormalities, Hydrocephalus, Polydactyly, Oesophageal atresia
- Cardiac abnormalities -situs inverses or dextrocardia ,Double outlet right ventricle, Pulmonary stenosis,VSD
- Skull deformities: Cranium bifidum, Microcephaly, Dolicocephaly
- TM joint: Anterior inferior displacement
- Cranial nerves involvement: I-X
- Pulmonary hypoplasia, obstructive sleep apnoea, laryngeal anomaly
- Renal abnormalities: Ectopic kidney
Severity of mandibular hypoplasia is graded as
- Grade I – Small mandible,normal shape,short ramus
- Grade II – Anteriorly and medially displaced TMJ, short and abnormally shaped ramus
- Grade III – Complete absence of mandibular ramus, no TMJ
The main challenge that we anticipated in this case was a difficult airway. We planned to go ahead with the left molar approach for tracheal intubation. The molar approach (4027773) of laryngoscopy is reported to improve glottic view in sporadic cases of difficulty laryngoscopy. In left molar approach laryngoscopy the blade is inserted from the left corner of the mouth at a point above the left molars. The tip of the blade is directed posteromedially along the groove between the tongue and the tonsil until the epiglottis and glottis come into sight. Before elevating the epiglottis, the tip of the blade is kept in the midline of vallecula and the blade is kept above the left molars to obtain the best glottic view. Previous authors have concluded that laryngeal view improved to Mallampatti Grade I (19419375) by the left molar approach in patients with simulated limited cervical movements, with a high success rate of tracheal intubation. If anaesthetist encounter an unexpected difficult airway, the left molar approach provides an easy and reliable option.
Conclusion
In Goldenhar Syndrome, anaesthetic management depends upon the challenge of gaining airway control and a safe conduit of anaesthesia by delineating the anaesthetic plan. In our case the vocal cords were visualized better by using the left molar approach. A good and vigilant post-operative care needs to be equally stressed. Identification of syndrome and associated abnormalities is very crucial in the management of such patients.