We are very happy to have received this contribution from our kind colleagues Drs. Subramanian and Sujith from Bangalore. Our thanks and sincerest apologies to them, in the hectic past weeks we oversaw having a contribution ( sadly enough, that doesn’t happen every day)
Anaesthetic management of Nance Horan syndrome for ophthalmic surgery
Sir,
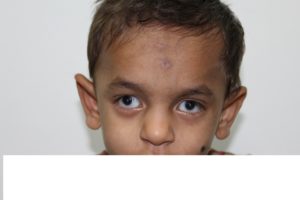
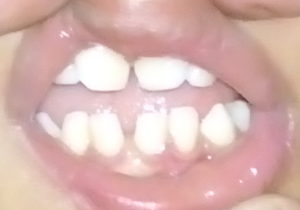
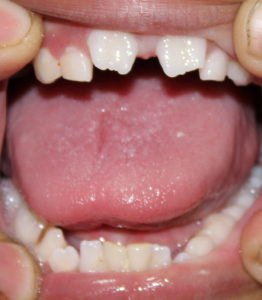
Two siblings, aged 3 and 7 years, both males and born of non consanguineous marriage were posted for congenital cataract surgery. Both were born full term with a birth weight of 3.5 kg. The 3 year old younger sibling was 13 kg in weight, 85 cm in height (5th percentile) with a head circumference of 41.5 cm. He had dysmorphic facies, brown hair, large protruding ears, microcephaly, global developmental delay and dental anomalies (Fig 1a-b). The elder sibling weighed 20 kg, was 118 cm in height (50th percentile) with a head circumference of 48 cm. He had microcephaly, dysmorphic facies with a long face, sparse brown hair and large pinna, Hutchinsonian teeth (small, widely spaced teeth with notch on the biting surface of incisors), carious teeth and short metacarpals. (Fig 2a-b) He was hyperactive and of subnormal intellect with delayed social and language milestones. Based on the above features, they were diagnosed to have Nance Horan syndrome. Both the brothers suffered from impaired vision since birth with white reflex in the eyes that had been neglected and were identified at a school health camp. The ocular diagnosis in both the brothers included bilateral congenital cataract, microcornea, deprivation nystagmus and bilateral amblyopia. An echocardiogram of the heart revealed a normal study. The brothers were posted for lens aspiration, posterior capsulorrhexis and anterior vitrectomy of the right eye. Examination of the airway revealed mild retrognathia. However mouth opening, jaw protrusion and neck extension were adequate.
There was no report in literature on anaesthetic challenges in Nance Horan syndrome. However, due to the presence of dental anomalies, a paediatric difficult airway cart was kept ready with age appropriate equipment. The younger sibling was anaesthetized using inhalation induction with sevoflurane in a mixture of air and oxygen. An intravenous line was secured and the child was given glycopyrrolate 0.1mg and Fentanyl 30µg. After ensuring adequate mask ventilation, neuromuscular blockade was achieved with atracurium 6 mg. After three minutes of mask ventilation, direct laryngoscopy was done with a Mac2 blade and it revealed a Cormack Lehane grade I view of the glottis and the trachea was intubated with a 5.0 mm internal diameter uncuffed endotracheal tube. The child was connected to the ventilator and anaesthesia was maintained with sevoflurane in a mixture of air and O2. Paracetamol 15mg/kg was administered for postoperative analgesia. The surgery lasted 45 minutes and at the end of surgery, neuromuscular blockade was reversed with and the trachea was extubated when the child was fully awake.
In the elder sibling, an intravenous line was secured after applying EMLA cream. Anaesthesia was induced with propofol 3mg/kg after premedication with glycopyrrolate 0.1mg and fentanyl 2µg/kg. Neuromuscular blockade was achieved with atracurium 10 mg once it was confirmed that mask ventilation was adequate. Direct laryngoscopy revealed a Cormack Lehane grade I view of the larynx and the trachea was intubated with a size 5.0 mm internal diameter cuffed endotracheal tube. He was connected to the ventilator on PCV mode with age appropriate ventilator parameters. Anaesthesia was maintained with sevoflurane in a mixture of air and O2 with paracetamol 15mg/kg intravenously for postoperative analgesia. The surgery lasted 40 minutes. NMB was reversed and the trachea was extubated when the child was awake. In both the children, the postoperative period was uneventful and the left eye was operated one month later.
Nance Horan syndrome (NHS) was first described independently by Nance and Horan in 1974 in the United States and Australia respectively.(1,2) There are just about 50 families worldwide who have been studied. One family of Asian Indian lineage with severe ocular findings has been mapped genetically.(3) It is otherwise called the cataract dental syndrome, mesiodens-catarct syndrome. The ophalmological and dental findings as well as the molecular and genetic analysis in NHS have been detailed expansively but the anaesthetic concerns have not been reported. The dental abnormalities include wide spacing between teeth (diastema), screw-driver or peg shaped central incisors, Hutchinsonian teeth, supernumerary incisors or posterior teeth and centrally located front tooth in the maxilla (mesiodens). The ophthalmological features include bilateral congenital cataract, microcornea, microphthalmia, nystagmus and strabismus. Facial dysmorphism with long face, large nose, high nasal bridge, prognathism and large anteverted pinna has been described. NHS is inherited as an X linked trait due to a mutation of the NHS gene on the short arm of chromosome 22. The NHS gene has been mapped to Xp22.13. All affected males manifest the ocular and dental features while carrier females show mild features but no intellectual impairment.(4)
The main anaesthetic concern would be with airway management as dental and ear anomalies are often associated with difficult airway. The differential diagnosis for NHS includes X-linked microphthalmia, Lenz syndrome, Oculo-facio-cardio-dental (OFCD) syndrome, and Oculo-cerebro-renal (Lowe) syndrome which are associated with airway abnormalities.(5) It is necessary that the age appropriate equipment for difficult airway be ready before administering anaesthesia. It is also likely that supernumerary teeth and retained deciduous teeth may hinder direct laryngoscopy or be prone to injury during laryngoscopy and intubation. The absence of hyperdontia or jaw anomalies made airway management smooth and uneventful in our case. Thus, we describe the management of anaesthesia in two siblings with NHS for bilateral cataract surgery.
References:
- Nance WE, Warburg M, Bixler D, Helveston EM. Congenital X-linked cataract, dental anomalies and brachymetacarpalia. Birth Defects Orig Art Ser. 1974; 10:285-91
- Horan MB, Billson FA. X-linked cataract and hutchinsonian teeth. Aust Paediatr J. 1974; 10:98–102.
- Vedam Lakshmi Ramprasad , Alka Thool, Sakthivel Murugan, Derek Nancarrow, Prateep Vyas, Srinivas Kamalakar Rao, Authiappan Vidhya, Krishnamoorthy Ravishankar, Govindasamy Kumaramanickavel; Truncating Mutation in theNHS Gene: Phenotypic Heterogeneity of Nance-Horan Syndrome in an Asian Indian Family. Ophthalmol. Vis. Sci. 2005; 46(1):17-23.
- Burdon KP, McKay JD, Sale MM, et al. Mutations in a novel gene, NHS, cause the pleiotrophic effects of Nance-Horan syndrome including severe congenital cataract, dental abnormalities, and mental retardation. Am J Hum Genet. 2003; 73:1120-1130.
- Toutain A. Nance-Horan syndrome.Orphanet, September 2007. Available at: http://www.orpha.net/consor/cgi-bin/OC_Exp.php?lng=EN&Expert=627.0 Accessed May 23, 2016.
Legend for the Figures:
Figure 1a, b show the facial(a) and dental(b) features of younger sibling
Figure 2 a, b show the facial (a) and dental (b) features of elder sibling
Title of the article: Anaesthetic management of Nance Horan syndrome for ophthalmic surgery
Contributors
- Subramanian Shalini, MD, Consultant Anaesthesia, Department of Anaesthesia, Narayana Nethralaya, NH Health city, Bommasandra, Bengaluru 560099
- CN Sujith , DNB, Consultant, Department of Anaesthesia, Narayana Nethralaya, NH Health city, Bommasandra, Bengaluru 560099
Department(s) and institution(s) : Department of Anaesthesia, Narayana Nethralaya, NH Health city, Bommasandra, Bengaluru 560099
Corresponding Author: Shalini Subramanian,
Phone: 07406610222
Email: [email protected]