From Chennai, India’s “Sankara Nethralaya-Eye hospital”, the following case-history was sent to us. Many thanks to Dr. Shobha Ravishankar, who has been supporting us with her case-stories from the beginning of the ROAH homepage!!!
Dr. Shobha Ravishankar1, Senior Consultant anaesthesiologist, Medical Research Foundation, Chennai. Dr. R. Kannan2, Senior Consultant anaesthesiologist, Medical Research Foundation, Chennai. Correspondance To: [email protected] Conflict Of Interest: Nil. Financial Interest: Nil.
Abstract
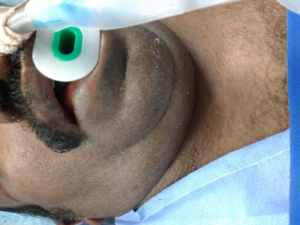
Klippel-Feil Syndrome (KFS) is known by the classic trait of short neck, limitation of neck movements and a low posterior hair line [Fig. 1 & 6]. Maurice Klippel and Andre Feil described the syndrome in 1912 (10.3406/bmsap.1912.8505 ). KFS has an incidence of 1:42,000 births and is one of the common congenital causes of difficult airway (10.3406/bmsap.1912.8505 )(4867516). The main anaesthetic challenge with these patients is a potential spine abnormality prone to an increased risk of neurological damage during airway Management (19299791).
Hence their anaesthetic management should be carefully planned keeping in mind the other abnormalities associated with this syndrome. We experienced a complete obstruction of endotracheal tube (ETT) due to blood clot during surgery. The management is discussed here.
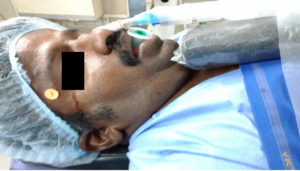
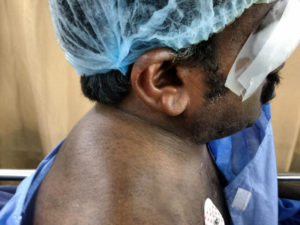
Keywords: Klippel-Feil syndrome, Short neck, Difficult airway, Blood clot blocking Endotracheal tube.
Case Report
A 24 year old male patient weighing 80kgs presented to our institution for penetrating keratoplasty III following a failed graft. This patient had lost his vision following trauma seven years ago. The patient had undergone cataract extraction with IOL, Trabeculectomy, Penetrating Keratoplasty twice (all surgeries under local anaesthesia) in some other hospitals. Blood investigations, ECG, ECHO were normal. X-ray of cervical spine showed the fused cervical vertebrae [Fig. 2]. CXR showed mild scoliosis, and tracheal displacement to left [Fig.3]. Preoperative vital parameters were unremarkable and airway examination revealed no neck extension with a Mallampati score III-IV.
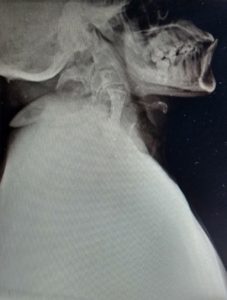
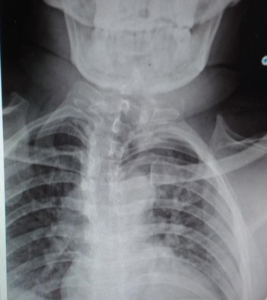
The patient was adequately fasted following universal fasting guidelines. As difficult intubation was anticipated our patient was prepared for awake fibro-optic intubation. The appropriate nostril was selected and was packed with local anaesthetic (2% lignocaine with adrenaline) and lignocaine gargle was also given to anaesthetise the pharynx. Routine monitoring protocols were followed. Patient was given 1.5mgs of midazolam, 0.5mcg/kg of fentanyl and 8mg of ondansetran I.V. at the beginning of the procedure inside the operating room. The chosen nasal cavity was well lubricated with 2% lignocaine jelly and the flexible bronchoscope with pre-threaded 6.5mm ID reinforced flexo metallic tube was negotiated. On visualisation of the vocal cords xylocaine spray was used and the scope was passed down the glottis. The tube was threaded down and its correct placement was checked by withdrawing scope, auscultation and capnography. There was a little bleeding in the nasal cavity during maneuvering which was cleared by suctioning. Patient was given an induction dose of propofol and cisatracurium 0.15mg/kg for muscle paralysis. Anaesthesia was maintained with oxygen, nitrous oxide and desflurane [Fig. 4]. The vital parameters remained stable. Total duration of the surgery was about one and half hours. Almost one hour into the surgery, the ventilator started displaying high airway pressure alarm. The circuit was checked for any obstructions/kinks but none were found. As EtCO2 started to touch around 50mmHg, manual ventilation was started. On auscultation, conducted sounds were heard. Inj. hydrocortisone 100mgs was given I.V. The SaO2 started to drop further and was about 92-93% and EtCO2 started to rise and was about 52-53mmHg. The surgeon was requested to patch the eye and all drapes were removed. On repeat auscultation, air entry was not heard on left hemithorax. Nitrous oxide and desflurane were discontinued and patient was ventilated manually with oxygen and sevoflurane (3%). Meanwhile, the oral cavity was suctioned and a sterile suction catheter was passed through ET tube. A blood clot was sucked out [Fig. 5] Air entry, SaO2, and bag compliance improved. EtCO2 also came down to 34-35 mmHg. Nitrous oxide and desflurane were reintroduced and surgeon was allowed to complete the surgery. At the end of the surgery residual neuromuscular paralysis was reversed and patient was extubated completely awake.

Discussion
Klippel-Feil syndrome is one of the congenital causes of difficult airway which occurs due to abnormal segmentation of the cervical somites in the third to eighth week of gestation (16153587). Out of the three variants of KFS, type 1 is an extensive abnormality in which several cervical and upper thoracic vertebrae are fused into a single block. In type 2 variant, failure of complete segmentation occurs at one or two cervical inter-spaces. Type 3 variant includes type 1 or 2 deformities with co-existing segmentation defects in lower thoracic or lumbar spine. Most common form is type 2 and it involves C2-3 and C5-6 interspaces. Other common anamolies associated with KFS include kyphoscoliosis, deafness, renal abnormalities, synkinesia, sprengels deformity and congenital heart disease (6747689)(10830068) Ventricular septal defect is the most common cardiac anamoly, occuring in 14-29% of the patients.
Endotracheal tube block due to various mechanical causes such as mucus, blood clot, dentures, kinking and external compression have been reported. Blockage of endotracheal or tracheostomy tube lumen can jeopardise ventilation and can be fatal (9925105)(15366320). Tight bag situation due to impaction resulting from blood clot within the airway causing oxygen desaturation was reported earlier (20885863). The sudden ETT block is difficult to anticipate or predict and may lead to panic. Blockage of ETT during intraoperative period is a possibility in difficult airway and thus the anaesthesia team should be prepared to take care of sudden airway blockade during conduct of anaesthesia. In manually ventilated patients, change in bag pressure alarms the anaesthetist to look for the cause of tight bag situation early, but during mechanical ventilation, the anaesthetist should be aware of the high pressure alarm incorporated in the anaesthesia work station.
To conclude, endobronchial blood clot can lead to sudden desaturation intraoperatively. There should be high index of suspicion of such a clinical presentation. Timely diagnosis and management can prevent catastrophic complications.
References
- Klippel M, Feil A. Un cas d’absence des vertebres cervicales. Soc Anat Paris Bull et Mem 1912; 14: 185.
- Gunderson CH, Greenspan RH, Glaser GH, Lubs HA. The Klippel Feil syndrome: genetic and clinical re-evaluation of cervical fusion. Medicine 1967; 46: 491-512.
- Khawaja OM, Reed JT, Shaefi S, Chitilian HV, Sandberg WS. Crisis resource management of the airway in a patient with Klippel Feil Syndrome, congenital deafness and aortic dissection. Anesth Analg 2009; 108: 1220-5.
- Kaplan KM, Spivak JM, Bendo JA. Embryology of the spine and associated congenital abnormalities. Spine J 2005; 5: 564-76.
- Nagib MG, Maxwell RE, Chou SN. Identification and management of high risk patients with Klippel Feil syndrome. J Neurosurg 1984; 61: 523-30.
- Chattopadhyay A, Shah AM, Kher A, Bharucha BA, Kharapurkar AP. Craniosynostosis and Klippel Feil syndrome: Its Association. Indian J Paediatr 1996; 63:819-22.
- Judson MA, Sahn SA. Airway obstruction arising from blood clot: three reports and review literature. Chest. 1999; 115: 292-300.
- Changjoo P, Hyunjeong K, Kwangwon Y. Acute obstruction of endotracheal tube: A case report. Anesth Prog.2004; 5: 62-4.
- Parthasarathy M, Ravishankar M. Tight bag. Indian J Anesth.2010; 54:193-8.